April 2021 Update
How are we managing our improvement project even during a major crisis?
Catherine Macrae, NBCP Scotland Project Lead
The first step our early adopter project leads took was to find out all of the professional groups they needed to engage with. We did this by working out who is involved in the journey a woman, partner or family makes during and after a loss during pregnancy or after birth - from the time when a concern is suspected right through to care in the community. Making connections with colleagues in those professions early on is vital because the key to meaningful and sustainable change lies with people. As Scotland’s National Clinical Director, Professor Jason Leitch, explains in this Open University talk that means building empowering and motivated change inside teams.
The next step was to review the quality and consistency of existing bereavement care against the 5 National Bereavement Care Pathways. Project leads found that in many ways good or excellent care was in place and the conversation could focus on how consistently that could be delivered by all staff and in all units and services. Leads were more confident about an accurate self-assessment if this conversation could take place with several staff directly delivering care. It takes more time to do this but gives scope to engage and motivate people.
Once the improvements needed are clear, leads could start to develop detailed project plans. They worked with colleagues to decide the effort needed for and likely impact of each improvement using an effort / impact grid.
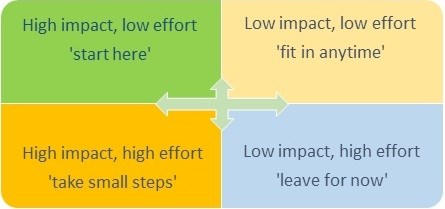
This task generates clear priorities and a sense of the right order to tackle changes in.
Being agile and learning from experience
Our approach to the project was always designed to be ‘agile’ – breaking improvement work into short stages of about 9 weeks and creating a detailed action plan only for the current stage. Achievements and blocks are reviewed at the end of each stage, so that we can learn what works to deliver change and what doesn’t. Our learning is then reflected in the new action plan. This flexible and reflective approach is really valuable in any project that encounters unexpected developments, which is often the case in my experience, and a pandemic is off the scale!
We need to keep at the centre of our thinking that we are piloting the Pathways with the aim of learning what is realistic and achievable. Our vision is that all healthcare professionals and staff who are involved in the care of a woman, partner or family are able to consistently deliver compassionate, person centred care. We are immensely grateful for the enthusiasm and commitment of our early adopter project leads throughout this challenging year.
